Working for long hours, no physical activity? Relying more on processed food? Feeling worried about diabetes? You’re not alone. According to global estimates over 537 million people were living with diabetes in 2021 and the number continues to rise. Awareness is increasing – but action starts now.
Diabetes mellitus: Key global facts
- The number of people living with diabetes worldwide has increased from approximately 198 million adults in 1990 to 828 million in 2022.
- Almost one in two adults (≈47%) with diabetes globally remain undiagnosed, representing about 252 million people aged 20–79 years.
- In 2024, diabetes caused over 3.4 million deaths (one every nine seconds).
- High blood glucose causes about 11% to 20% of all cardiovascular deaths globally.
- Diabetes is a leading cause of renal (kidney) failure.
- Diabetes mellitus is the leading cause for nontraumatic (without any external injury) lower extremity amputation.
According to the International Diabetes Federation, the global diabetes burden is expected to escalate dramatically, reaching an estimated 853 million adults by 2050.

So, what is diabetes?
Diabetes is a condition where your body struggles to control blood sugar levels, which leads to too much sugar building up in the bloodstream.
Let’s talk about the different types of diabetes mellitus.
There are varieties of diabetes mellitus (DM). But the most important ones are:
- Type 1 diabetes mellitus results from an absolute deficiency of insulin due to failure of pancreatic insulin production and typically presents in childhood or adolescence.
- Type 2 diabetes mellitus is characterized by insulin resistance, often accompanied by
a relative insulin deficiency, and most commonly affects adults, though its incidence in younger individuals is rising.
- Gestational diabetes mellitus develops during pregnancy and pregnancy related hormones cause insulin resistance, leading to high glucose level in blood.
(Note: Insulin is required for utilization of glucose in the body.)
Here are some most common symptoms of Diabetes
There are some common symptoms through which diabetes may first make itself evident.
Symptoms
- Frequent urination
- Increased thirst and dry mouth
- Increased appetite – feeling hungry after meals
- Delayed wound healing
- Sudden weight gain or drop
- Numbness or tingling sensations in hand or feet
- Blurred vision
- Fatigue and dizziness
- Irritability

Many of us think we can handle these issues on our own and wonder why we should consult a doctor for such “small” problems. This mindset, common among us Indians, often leads to neglecting early warning signs. But neglecting these early symptoms may cost your beautiful and peaceful life in future. So, what are the complications it might lead to?
Complications
Diabetes can lead to acute (sudden and severe) and long-term complications, mainly due to increased blood sugar levels.
Acute diabetic complications:
- Diabetic ketoacidosis usually occurs in type 1 diabetic patients, if the glucose in our body is not utilized due to insulin deficiency, the body breaks down fat for energy which leads to production of harmful acids( ketones), leading to dehydration, nausea, vomiting, and even coma if untreated.
- Hyperosmolar hyperglycemic state is usually seen in type 2 diabetic patients. When your blood sugar level is very high ( i.e > 600 mg/dl ) over a long period of time it leads to severe dehydration and your blood becomes thick and concentrated. It requires immediate medical treatment.
- Hypoglycemia is most commonly seen in patients who are diabetic and are on insulin or oral hypoglycemic drugs. Severe hypoglycemia is very low blood sugar and the symptoms may include sweating, anxiety, confusion, dizziness, seizures.
Long term diabetic complications:
Untreated high blood glucose levels can gradually damage blood vessels and nerves, affecting multiple organs over time. Unlike acute complications, these changes develop silently and often become noticeable only after significant damage has already occurred. Long-term complications can be broadly classified as microvascular and macrovascular and other complications.
Microvascular complications (damage to small blood vessels)
These affect organs that depend on tiny blood vessels
- Eye problems
- Diabetic retinopathy– Damage to blood vessels of the retina → causes blurred vision or blindness.
- Macular edema– Swelling of the central part of the retina → difficulty in seeing.
- Nerve damage (Neuropathy)
- Tingling sensation, numbness, burning pain
- Loss of sensation in feet → unnoticed wounds → ulcers and infections
- Kidney damage (Nephropathy)
- Kidneys slowly lose their filtering ability.
- Can lead to kidney failure requiring dialysis.
Macrovascular complications (Damage to large blood vessels)
These affect major blood vessels supplying the heart, brain, and limbs.
- Heart disease
- Increased risk of heart attack
- Can also lead to heart failure
- Poor blood flow to legs
- Causes leg pain while walking, slow wound healing.
- Brain involvement
- Increased risk of stroke
- Memory problems over time
Other long- term complications
These occur due to nerve damage, poor blood flow, and weak immunity
- Gastroparesis – Slow stomach emptying → nausea (unpleasant sensation of wanting to vomit)
- Diarrhea
- Diabetic foot ulcers (~14–24% people with foot ulcer need amputation)
- Sexual dysfunction (erectile dysfunction in men)
- Cataracts
- Glaucoma – Increased eye pressure damaging vision
- Hearing loss
- Frequent skin infections
Unmanaged gestational diabetes can lead to problems that can affect both mother and child.
Complications affecting the child an include:
- Premature birth
- High birth weight
- Increased risk of type two diabetes in later life
- Low blood sugar
- Jaundice
- Still birth
These are serious, life threatening complications, and feeling worried is a natural human response. However, most of these long-term complications can be prevented or delayed with good diabetes management and regular follow-up.
Can you prevent diabetes?
“Prevention is better than cure” is a phrase we hear often, yet its true value is realized only when it is practiced consistently. Type I diabetes cannot be prevented because it is an autoimmune condition and Type II diabetes is preventable and manageable.
Preventive measures for Type II diabetes mellitus
- Maintain normal blood pressure
- Quit smoking and avoid tobacco
- Exercise regularly (walking, cycling, sports)
- Eat a balance diet; avoid excess sugar and junk food
- Maintain healthy body weight
- Get adequate sleep and manage stress
- Avoid alcohol consumption
- Go for regular health check-ups
- Monitor blood sugar level, especially if at risk.

Prevention of complications
Diabetic Retinopathy
The most effective therapy for diabetic retinopathy is prevention. Intensive glycemic and blood pressure control will delay the development and slow the progression of retinopathy in individuals with either type I or type II Diabetes Mellitus.
Women with type I or type II Diabetes Mellitus who are planning pregnancy should be screened prior to pregnancy and during pregnancy.
Diabetic Nephropathy
The optimal therapy for diabetic nephropathy is prevention by control of blood glucose and blood pressure ( blood pressure < 130 / 80 mmHg ).
Diabetic Neuropathy
Prevention of diabetic neuropathy is critical through improved glycemic control. Lifestyle modifications have some impact in some conditions of neuropathy.
Greater body mass index (BMI) and smoking increases the risk of neuropathy.
Cardiovascular diseases
Cardiovascular diseases are twice as common in individuals with diabetics and worse than for nondiabetics.
Lifestyle modifications play a crucial role and it includes maintaining good lipid profile, regular workout, smoking cessation, adequate amount of sleep and stress management.
Diabetic foot ulcer
Diabetic foot ulcers are serious complications of diabetics and are the leading cause of amputations of foot or leg. They occur in combination of neuropathy and vascular diseases.

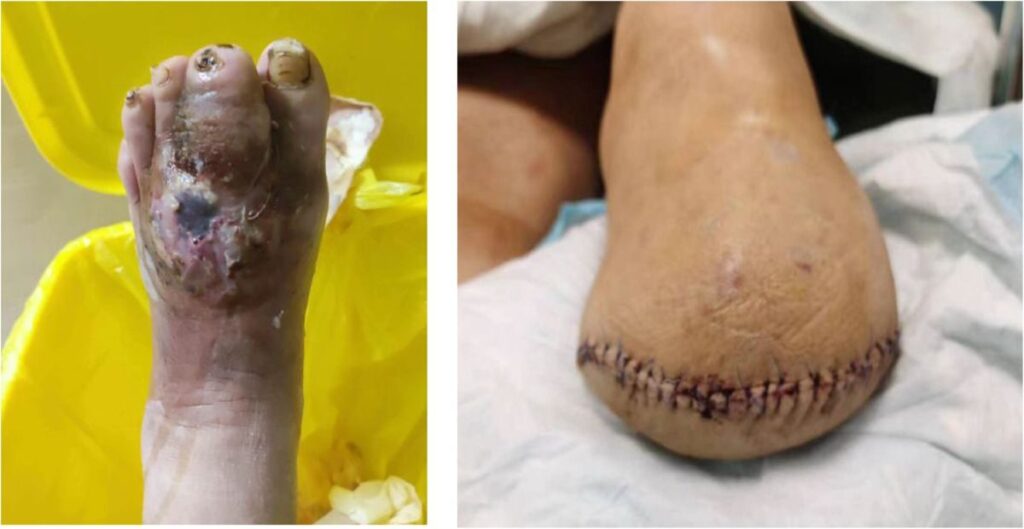
The most effective measures to prevent it are:
- Regular blood glucose monitoring and keeping it in normal range
- Daily check your feet for cuts, blisters, redness and swelling
- Wash and dry your feet properly, especially in between toes
- Wear diabetic footwear, and avoid walking barefoot.
How is diabetes diagnosed?
Screening tests includes:
- Fasting Plasma Glucose (FPG)
Measures blood sugar after at least 8 hours of fasting.
- Random Plasma Glucose (RPG)
Blood sugar is measured at any time of the day.
- Oral Glucose Tolerance Test (OGTT)
Measures blood sugar before and 2 hours after drinking a glucose solution.
Commonly used in pregnancy.
- HbA1c (Glycated hemoglobin)
Reflects average blood glucose levels over the past 2-3 months.
- Urine Glucose Test
Used only for screening, not used for diagnosis
Presence of glucose in urine may suggest high blood sugar.
Management and treatment
Already suffering from diabetes? There are millions of people suffering from diabetes, yet leading a normal life with proper management.
Lifestyle management
Nutritional Recommendations
Fat in diet
- Prefer a diet rich in monounsaturated and polyunsaturated fatty acids.
- Limit saturated fats.
- Minimal or no trans fat consumption.
Carbohydrate in diet
- Monitor carbohydrate intake according to calorie needs
- Maintain consistent carbohydrate distribution across meals
- Minimize consumption of beverages and foods with added sugar
Physical Activity
Regular physical activity improves the insulin sensitivity in your body and helps control blood glucose level. At least 150 min/week of moderate exercise is recommended.
Benefits of regular exercise
- Increases insulin sensitivity in your body
- Reduces cardiovascular risk
- Helps to maintain lower blood pressure
- Helps to maintain muscle mass
- Reduces body fat and support weight loss
- Improves mental state of your body.
Note: To avoid exercise related hyper- or hypoglycemia, individuals with Type I diabetes mellitus should
- Monitor blood glucose before, during and after exercise
- Delay exercise if blood glucose more than usual and if ketones are present
- If blood glucose less than usual, ingest carbohydrate before exercising as needed to prevent hypoglycemia
- Decrease insulin dose (based on previous experience) before and after exercise and inject insulin into a nonexercising area
- Learn individual glucose response to different types of exercise.
Mental health management
Individuals living with diabetes mellitus affect their daily life and their psychosocial aspect.
Blood sugar levels can be influenced by factors such as – Stress, Illness, Hormonal changes etc. According to the American Diabetes Association defines diabetes distress as – Negative psychological reactions caused by the emotional burden of living with and managing diabetes.
This includes:
- Feeling overwhelmed
- Burnout from constant monitoring
- Fear of complications
- Frustration with fluctuating glucose levels.
This is not depression, but it can lead to depression.
How does emotional stress affect diabetes control?
It causes poor adherence to:
- Diet plan
- Exercise routines
- Monitoring schedules
- Irregular eating patterns
- Skipping self care activities.
How to manage it?
- Manage stress by involving yourself in relaxing techniques such as yoga, meditation etc
- Get adequate amount of sleep and maintain regular sleep schedule
- Seek emotional support from your families, friends and support groups.
Core management
Glycemic and metabolic management
Type I diabetes mellitus
Individuals with Type I diabetes mellitus partially or completely lack insulin production.
In this condition the main goal is to implement an insulin therapy approach that mimics physiologic insulin secretion.
Therefore, life-long insulin therapy is a must for survival and effective glycemic control.
Type II diabetes mellitus
In this condition the goal of glucose directed therapy for Type II diabetes mellitus is similar to those in Type I diabetes mellitus, but here it is individualized for each patient. The management includes the usage of Glucose -Lowering agents, Insulin secretors, Inhibitors etc.
The treatment also includes management of obesity, hypertension.
Diabetic ketoacidosis and Hyperosmolar Hyperglycemic state
These are diabetic medical emergencies and require immediate hospitalization. The management includes Fluid replacement, Insulin therapy, Electrolyte correction. Treatment of diabetic emergencies at home is not advised and it’s highly unsafe.
Hypoglycemia
It requires immediate restoration of glucose levels to a safer range. It includes oral intake of oral glucose or sugary drinks.
Hypertension
Many individuals with type I and type II diabetes mellitus develop hypertension.
It accelerates complications of diabetes mellitus, particularly cardiovascular diseases, nephropathy, and retinopathy.
Higher blood pressure often requires more than one medication under medical supervision.
In pregnant women with diabetes and long standing hypertension, blood pressure control is associated with better pregnancy outcomes.
Support system
Care
Proper medical care is essential for effective diabetes management. Regular follow-ups with healthcare professionals help in monitoring blood sugar levels, detecting complications early, and receiving appropriate guidance.
Community
Support from family, friends, and peers plays a vital role in daily diabetes care. Encouragement from loved ones helps individuals follow healthy routines, while interaction with others living with diabetes provides shared experiences, motivation, and practical coping strategies.
Technology
Technology has become an important support tool in diabetes management. Blood glucose monitoring devices, mobile health applications, reminders, and educational resources help individuals track their health, improve adherence, and make lifestyle much more easier.
Conclusion: Living with diabetes
Living with diabetes should not break your heart and soul, one should take it positively and focus on the aspects where you can control it. With the right mindset diabetes becomes a part of your life, not a barrier.
References:
- Diabetes Mellitus : Diagnosis, Classification, Pathophysiology, Management, therapies and complications: Harrison’s – Principles of internal medicine [22nd edition].
- Diabetes Mellitus: Park’s Textbook of preventive and social medicine.
- Diabetes: World health organization.[https://www.who.int/]
- Diabetes: Cleveland clinic.[https://my.clevelandclinic.org/]
- Stabley JN, Towler DA. Arterial Calcification in Diabetes Mellitus: Preclinical Models and Translational Implications. Arterioscler Thromb Vasc Biol. 2017 Feb;37(2):205-217. doi: 10.1161/ATVBAHA.116.306258. Epub 2016 Dec 22. PMID: 28062508; PMCID: PMC5480317..[pubmed]
- Müssig K. Schwer einstellbarer Diabetes: Was steckt dahinter? [Difficult-to-control diabetes]. MMW Fortschr Med. 2025 Apr;167(6):52-55. German. doi: 10.1007/s15006-025-4756-3. PMID: 40180741.[pubmed]
- Diabetic foot ulcer image 1: https://punefootankle.com/midfoot-and-forefoot-treatment-pune/diabetic-foot-ulcers/
- Diabetic foot ulcer amputation image 2: https://www.nature.com/articles/s41598-024-78215-7.


