Many women fear the word cervical cancer but on the other hand they lack awareness about the disease There is a lot of stigma and shame attached to this disease, women are hesitant to approach a doctor at the right time. Even men need to know about the disease as the virus responsible for this cervical cancer can also affect them with other cancers. It’s high time both girls and boys receive the vaccine and contribute towards elimination of the disease.
Hope this article would be instrumental in breaking all the barriers and enlighten both men and women about the cause, prevention and early detection of cervical cancer
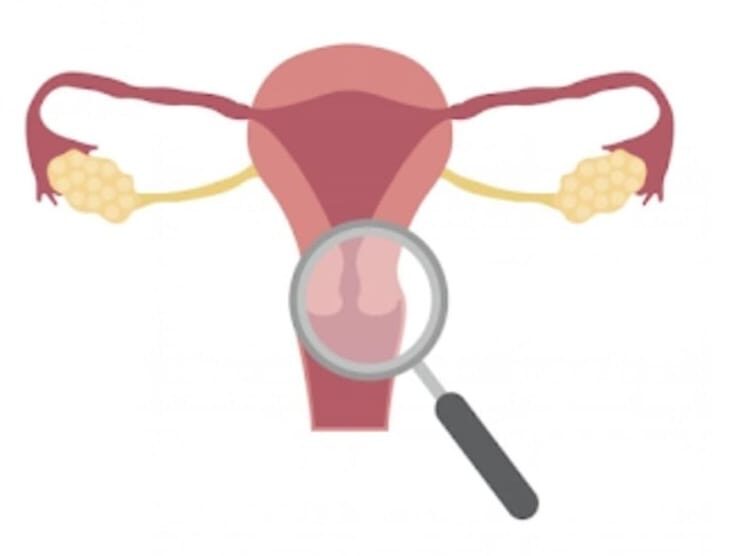
What is cervix ?
The cervix is the lowermost narrow part of the uterus that opens into the vagina. Cervix regulates the passage of sperm, allows menstrual blood to flow out during menstruation, during pregnancy it remains closed and firm to protect and support the fetus, and during labour it dilates and allows delivery of the baby.
What is cervical cancer ?
All organs are made up of cells. Development of abnormal cells within the cervix followed by uncontrolled multiplication and spread of these abnormal cells leads to cervical cancer. It is the second most common cancer among females in India. It is caused by Human Papilloma Virus infection.
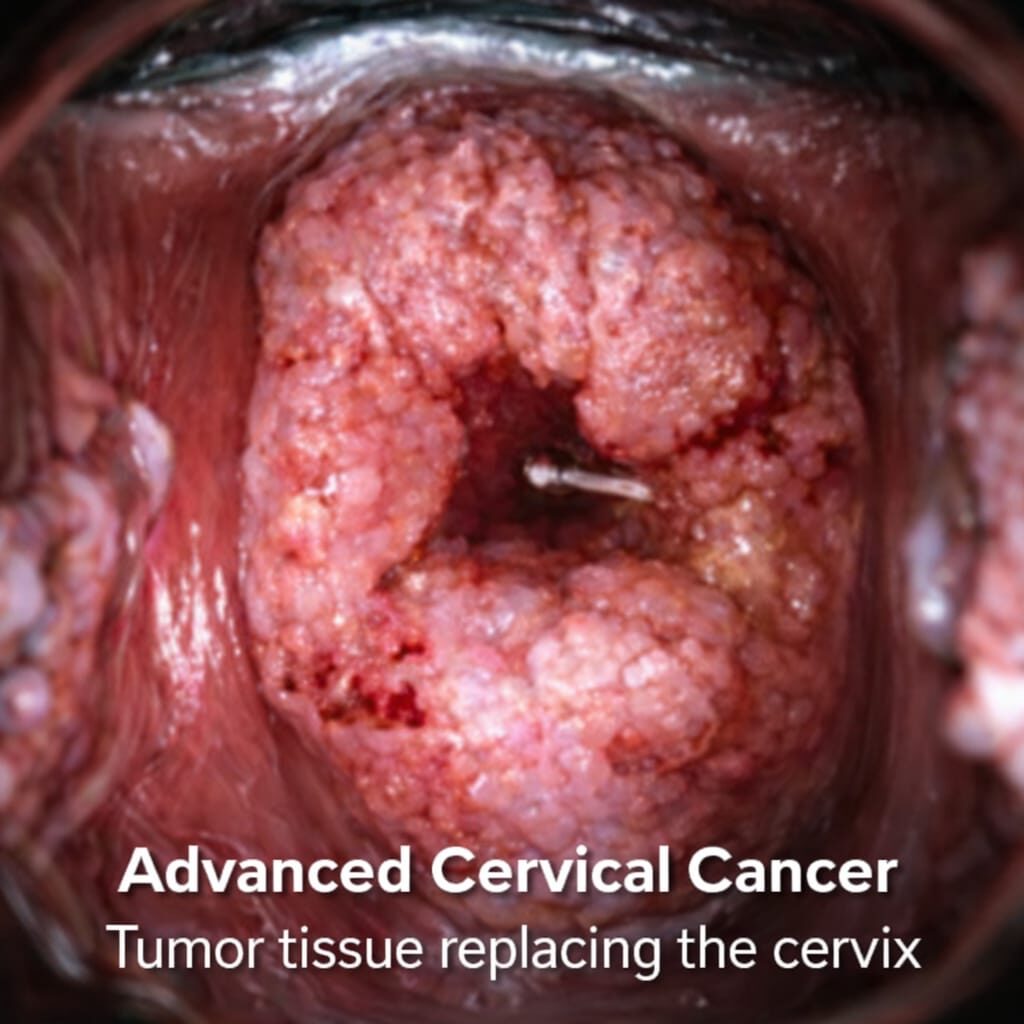
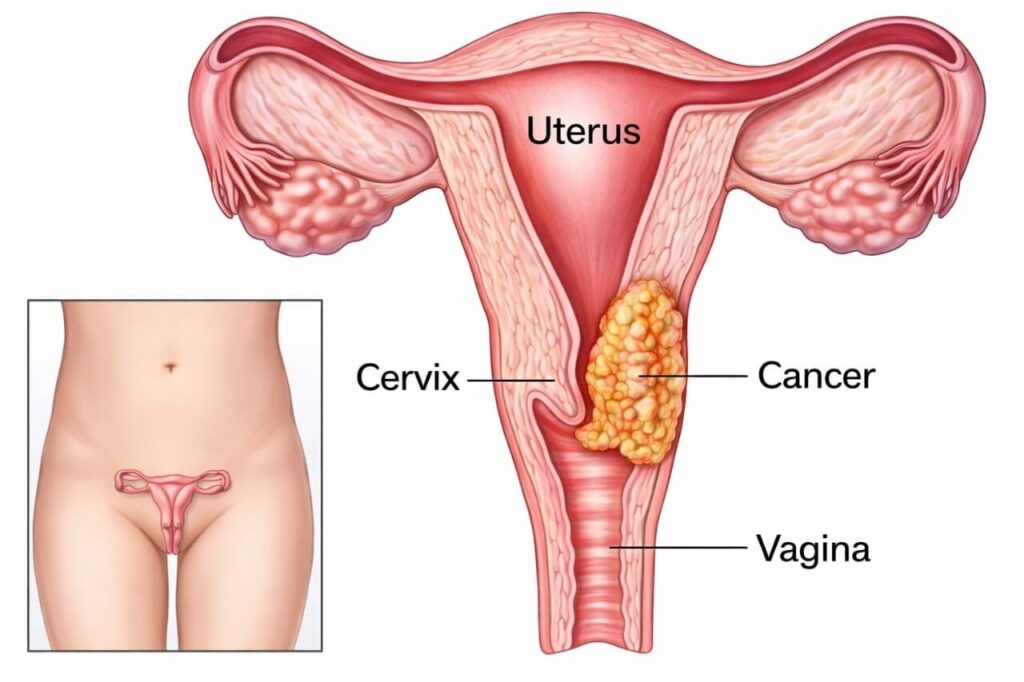
Cause for Cervical Cancer
Human Papilloma Virus (HPV) is the most common viral infection of the reproductive tract responsible for development of cervical cancer. There are several strains of HPV that have a high potential of causing cervical cancer and these are called as high risk types which are 16, 18, 31, 33, 45, 52 and 58. There are several other HPV types which have a low potential to cause cervical cancer and these are called low risk types. HPV infection causes a range of conditions affecting both men and women. In women it is responsible for cervical, vaginal, vulval, anal, oropharyngeal cancers and genital warts . In men it may cause cancers of the head, neck, oropharynx (throat and base of tongue/tonsils) anal, penile cancers as well as anogenital warts.
One should note that 70-90 % of women acquire HPV infection in their life time but not all of them develop cervical cancer as most of the women with good immunity recover from this HPV infection spontaneously but a small percentage of women have persisting HPV infection for years, these women when not identified and treated predisposes to the development of cervical cancer.
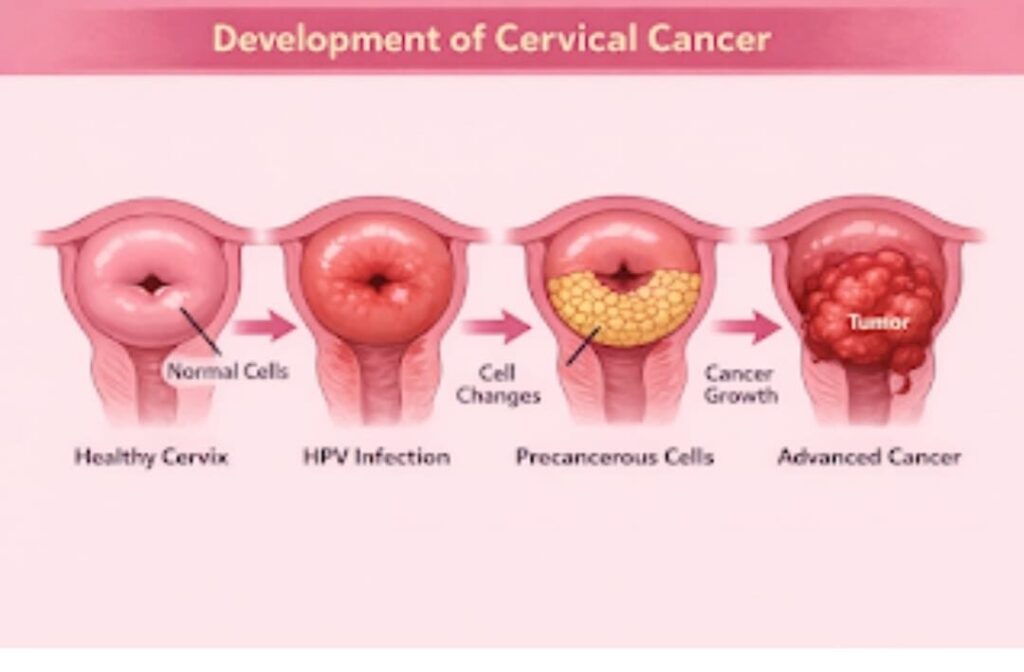
Risk factors contributing to persistence of HPV infection
- Early age of sexual activity
- Multiple sexual partners
- High risk sexual partner
- Smoking and alcohol use
- Immunosuppression
- Chronic cervicitis (repeated infection of the cervix)
- Low socioeconomic status
- Early child bearing
- Multiple pregnancies
Burden of cervical cancer in India
Cervical cancer is a major public health problem in India. It is the second most common gynaecological malignancy among Indian women aged 25-44 years and is the leading cause of mortality among women with an incidence of 3.5% . It is estimated that one woman in India dies every 8 mins from cervical cancer.
As per 2020 statistics in India, the number of new cases was 123,007 and deaths due to cancer cervix were estimated at 77,348, and the 5-year prevalence was 283,842. An estimated 604,000 women were diagnosed with cancer cervix worldwide, with India contributing to almost one-fourth of the global burden of cervical cancers indicating a very high incidence among Indian women and need for immediate intervention.
World Health Organisation’s (WHO) goal for elimination of cervical cancer
It is very crucial to understand that by preventing HPV infection through early vaccination in teenage girls, early detection of women with HPV infection and precancerous lesions, following them with appropriate monitoring and treatment can eradicate cervical cancer from this world.
WHO in 2020 launched a global strategy to accelerate the elimination of cervical cancer by 2030 with the following targets :
- 90% of girls fully vaccinated with HPV vaccine by age 15 years
- 70% of women are screened with a high-performance test by 35 years of age and again by 45 years of age
- 90% of women identified with cervical disease receive treatment (90% of women with precancer and invasive cancer managed).
Warning signs of cervical cancer
- Per vaginal bleeding ( bleeding through the vagina) in between cycles
- Bleeding after intercourse
- Foul smelling vaginal discharge
- Bleeding per vagina after attaining menopause
These symptoms are a warning that you may have acquired cervical cancer or cervical infection and hence you need an immediate examination and evaluation by a Gynaecologist. Do not panic if you are experiencing these symptoms as other conditions can also mimic them, but make sure to consult a Gynaecologist immediately for proper evaluation, accurate diagnosis and appropriate treatment.
As prevention is better than cure it is recommended that all women take preventive measures prior to development of these symptoms.
Prevention
- Primary prevention: It involves actions taken to stop the disease before it starts by targeting healthy individuals, by reducing risk factors, and promoting healthy lifestyles.
This includes:
- Education and health awareness: Various awareness camps should be held by health care professionals to educate people about the risk factors and prevention via vaccines. Lack of awareness leads to myths, stigma, fear, and reluctance among people, by education, individuals can take confident steps towards safeguarding women’s health.
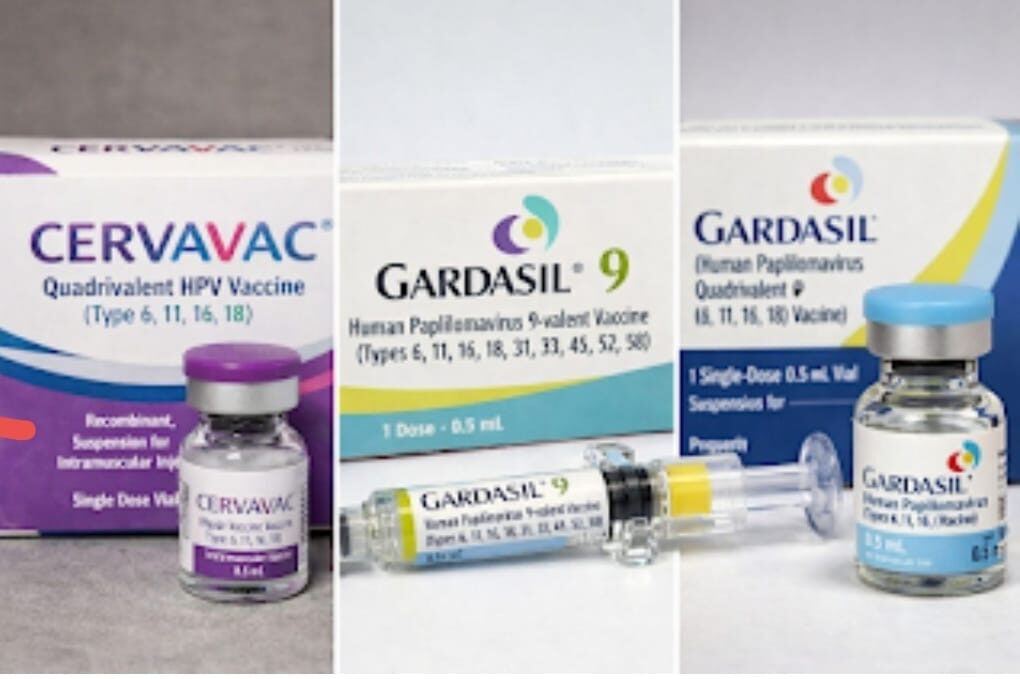
- HPV vaccinations – It is a reliable method to prevent cervical cancer.It includes quadrivalent vaccine (Cervavac and Gardasil) which covers 4 HPV strains and nanovalent vaccine (Gardasil 9) which covers 9 HPV strains. These vaccines also prevent genital warts.
Government of India has introduced Cervavac into its universal immunization program targeting girls for cervical cancer prevention along with screening programs to meet WHO goals.
Vaccine schedule as per FOGSI- ICOG guidelines:
| Schedule | |
| Optimal dose – girls | 9 -14 years : Two doses at least 6 months apart 15 -26 years : Three doses (0, 1 – 2 months, 6 months) Three doses for older women till 45 years, Regular screening as per guidelines has to be followed in the reproductive age group |
| Boys | Boys can be vaccinated from 9–26 years 9–14 years: 2 doses 0, 6 months 15–26 years: 3 doses 0, 2, 6 months |
- Secondary prevention: It focuses on early detection and prompt treatment of existing conditions before they cause severe symptoms or complications, aiming to halt progression and reduce impact. All screening tests for cervical cancer provide secondary prevention.
This includes:
- VIA (visual inspection by acetic acid)
- VILI ( visual inspection by lugol’s iodine)
- Pap smear
- LBC(liquid based cytology)
- Primary HPV testing
VIA and VILI are simple cervical cancer screening methods which can be done even in the periphery with low resource settings (no need for labs or advanced equipments), its cost effective, requires only basic equipments, can be done by health workers with brief training, it provides immediate results allowing immediate treatment for positive cases (see and treat). These tests facilitate screening of large populations quickly and are beneficial in high burden areas.
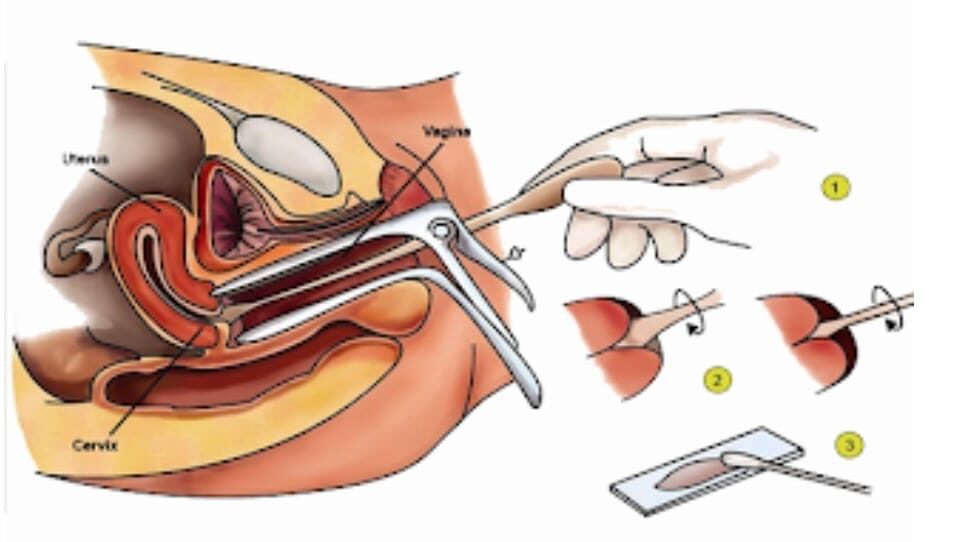
PAP Smear : Also called as Pap test.
- The most common and important screening test for cervical cancer.
- This test can detect abnormal cells in your cervix which are cancerous and also the cells that have the potential to become cancerous.
How is the test done: It is usually done by a gynaecologist in an outpatient setting. Cervix naturally exfoliates cells and sheds them regularly, these shed cells are collected with the help of a swap or brush and smeared on a slide which then is sent to the lab for analysis.
LBC: it is similar to pap smear but here the shed cells are collected in a liquid medium. This is more accurate than the pap test as it removes blood/ mucus allowing for better cell visualization. It is also useful in HPV DNA testing.
Primary HPV testing: It is a highly sensitive screening method that uses DNA test to detect high risk HPV types. A positive HPV test means a high risk type of HPV was found in your cervical cells, but it does not necessarily mean you have cervical cancer so further testing to rule out precancerous and cancerous lesions are needed like Pap smear or Colposcopy
When both HPV DNA testing and LBC are done together it is called as cotesting.
How frequently should you undergo screening?
Screening should start at the age of 30 years.
If primary HPV testing is the choice of screening, then it has to be done once in 5 years.
If Pap smear, VIA, VILI, LBC is the choice of screening, then it has to be done once in 3 years.
An individual aged 65 years or more with consistent negative screening since the last 15 years can exit screening.
Why should boys take HPV vaccination
– HPV vaccine protects boys from acquiring oropharyngeal, penile cancers.
– HPV vaccine protects boys against genital warts.
– Taking the vaccination also prevents transmission to future sexual partners.
– Widespread vaccination contributes to overall community protection by reducing circulation of the virus (herd immunity).
– It is proven to be safe and effective.
Vaccinating boys is a crucial step taken towards reducing the burden of cancer caused by HPV globally
Some common myths attached to HPV vaccine
- HPV vaccine causes infertility: There is no evidence that HPV vaccines affect infertility. Large studies show normal pregnancy rates in vaccinated individuals. Therefore the vaccine does not impair fertility or cause any kind of complications during pregnancy
- HPV vaccine encourages early sexual activity: Many studies show no increase in sexual behaviour after the vaccine. The vaccine is given only for better immune response and not to provide sexual activity
- Only girls need HPV vaccination: HPV can affect both males and females so it is crucial to vaccinate both genders to avoid certain cancers
- HPV vaccine causes cancer: Vaccine contains virus like particles but not the live virus, therefore it cannot cause cancer or HPV infection
- HPV vaccines have serious side effects: HPV vaccines are extremely safe. Some common side effects seen after the vaccination are pain at the site of injection, mild fever and headache which are common side effects for most of the vaccinations
- HPV vaccine is unnecessary if a person is not sexually active: The vaccine works best when given before exposure to the virus, therefore it is recommended to take the vaccine before sexual debut
- HPV vaccine gives 100% protection against cervical cancer: The quadrivalent vaccine protects against high risk HPV types 16 and 18 which causes 70-80% of the cancers.Nanovalent vaccine protects against high risk HPV types 16, 18, 31, 33, 45 52 and 58 which are responsible for 90-93% of cervical cancers but does not provide protection against all HPV types, hence regular screening is still required even after vaccination.
- HPV vaccine is new and not well studied: It is in use since 2006, with hundreds of millions of doses administered worldwide with extensive safety data
- HPV vaccine is only for teenagers: The vaccination can be taken beyond teenage but the efficacy of the vaccine is maximum when taken between 9 to 14 years
- HPV vaccine can treat existing HPV infections: The vaccine is preventive and not therapeutic, therefore it does not cure existing HPV infection
Take home message
Cervical cancer is completely a preventable cancer. With availability of effective HPV vaccination, simple and reliable screening methods and increasing public awareness, the burden of this disease can be reduced drastically. Preventive measures are safe, evidence based and accessible and when adopted early, they offer life long protection. With collective efforts of healthcare providers, policy makers and the public , the vision of a future where cervical cancer is rare and ultimately eliminated sounds realistic and achievable. Let us all join hands towards the mission of eliminating cervical cancer from this world.
REFERENCES
- Cervical cancer – WHO Dec 2 2025: https://www.who.int/news-room/fact-sheets/detail/cervical-cancer
- FOGSI-ICOG Good Clinical Practice Recommendations (GCPR) Prevention and Management of Cervical Cancer: https://www.fogsi.org/wp-content/uploads/2024/06/GCPR-Cervical-Cancer-18th-June-2024.pdf
- https://www.cdc.gov/vaccines/vpd/hpv/hcp/recommendations.html
- WHO – Cervical cancer elimination initiative: https://www.who.int/initiatives/cervical-cancer-elimination-initiative
- WHO- Global strategy to accelerate the elimination of cervical cancer as a public health problem: https://www.who.int/publications/b/55745
- FOGSI- UNICEF presents for every child July 2024 Models used for illustrative purposes only “A Guide Book for Master Trainers: Preventing Cervical Cancer through through HPV Vaccination in India”: https://www.fogsi.org/wp-content/uploads/2024/07/HPV-VACINATION-1.pdf


