Sometime in the late 20th century, the developed world realized it had a massive problem with sugar. It wasn’t a loud announcement at first but a slow realization spurred by the numbers: obesity rates were climbing, metabolic diseases like Type 2 Diabetes and fatty liver (NAFLD) weren’t just medical curiosities anymore; they were everywhere, it was a very real silent pandemic crippling metabolisms across the population.
Eventually, the finger pointed squarely at sucrose-which is nothing but common table sugar. Sugar wasn’t just a dietary indulgence; it was driving a public health disaster. This triggered a genuine “sugar panic” inside the big food and beverage companies. They were staring at a hole in the market that threatened their bottom line.
Society ended up in a weird paradox. On one side, we were hooked on hyper-palatable, sweet, energy-dense foods—decades of industrial processing and culture had made sure of that. But on the flip side, we were terrified of the consequences: the weight gain, the insulin resistance, the chronic sickness.
We needed a fix, and fast. Everyone—from the average shopper to the food giants—was looking for a transformative solution. The goal was simple but difficult: keep the modern convenience and intense flavour we loved, but strip away the physiological price tag.
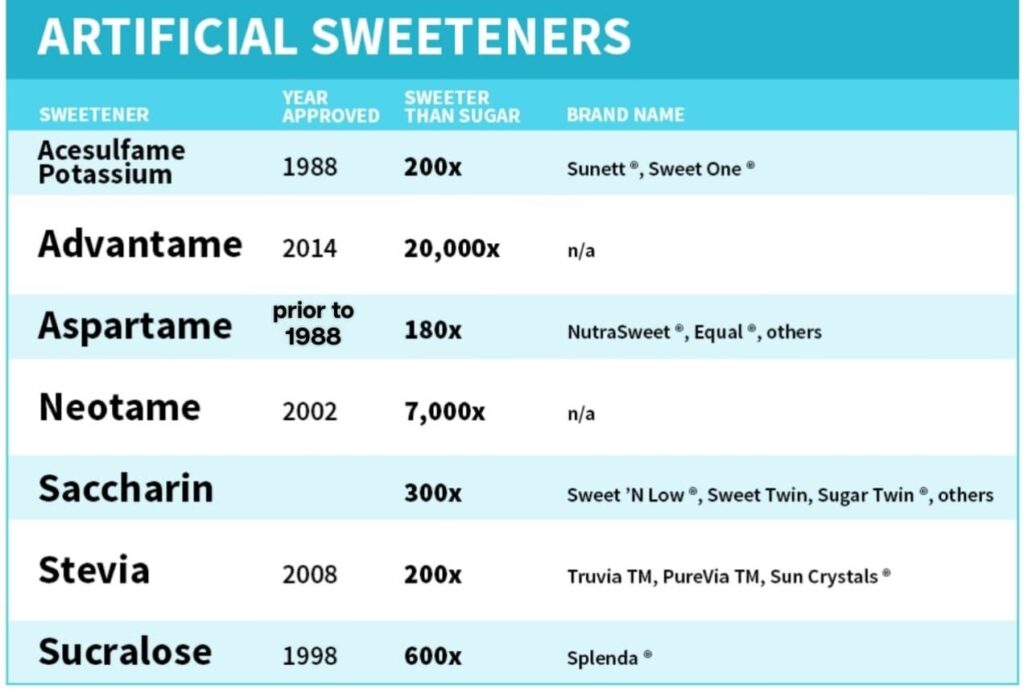
What Are Artificial Sweeteners?
At their fundamental level, artificial sweeteners, clinically known as non-nutritive sweeteners (NNS), are chemical mimics. They are synthetic or semi-synthetic molecules engineered to hijack the body’s taste receptors, offering an intensity of sweetness often hundreds or thousands of times more potent than table sugar. They are termed “non-nutritive” because the human body handles them in one of two ways: either it lacks the enzymatic machinery to metabolize them, allowing them to pass through the system unchanged, or they are so potent that they are required in such minute quantities that their caloric load is statistically irrelevant.
The development of these compounds was initially driven by a noble medical necessity: the management of diabetes. By decoupling the sensation of sweetness from the spike of glucose, scientists hoped to allow diabetics to enjoy palatable foods without immediate glycemic danger. However, there is a fundamental difference between these synthetic agents and natural sugars. Natural sweeteners like sucrose or fructose act as both fuel and flavor; they tell the brain that energy has arrived. Artificial sweeteners are purely signaling agents. This creates a biological mismatch known as the Sweet Taste–Calorie Disconnect.
Evolution trained our brains over millions of years to recognize “sweet” as a reliable signal for “incoming energy.” Artificial sweeteners trigger this signal but provide no fuel, essentially crying wolf. The prevailing hypothesis suggests that repeated false alarms may eventually lead the body to stop preparing for sugar intake properly, potentially contributing to metabolic confusion. However, metabolic confusion here can be an arbitrary term, for it might not directly translate to weight gain, it however also shouldn’t understate the harm of natural sugar. We simply need more study on the actual comparative harm/benefit ratio of these substances.
The Landscape of Synthetic Sweetness

The modern food landscape is dominated by a few key players, each with unique chemical profiles and histories. Aspartame is perhaps the most ubiquitous, lining the shelves of diet sodas and tabletop packets. Chemically, it is a methyl ester of the aspartic acid and phenylalanine dipeptide. Because it breaks down under heat, it is rarely used in baking, and it carries a specific warning for individuals with Phenylketonuria (PKU), who cannot metabolize phenylalanine. Sucralose represents a different approach; it is essentially a sucrose molecule that has been selectively chlorinated. By replacing three hydroxyl groups with chlorine atoms, the molecule becomes unrecognizable to the body as fuel while remaining heat-stable, making it the sweetener of choice for baking and industrial cooking.
The old guard is represented by Saccharin, a sulfonamide-based compound discovered in the late 19th century. Despite a rocky history involving controversy over bladder cancer in rats—findings that were later deemed irrelevant to human biology—it remains a staple in the industry. Acesulfame Potassium (Ace-K) is frequently used in synergistic blends to mask the bitter aftertastes inherent in other sweeteners. Interestingly, the case of Cyclamates offers a window into the complexity of global regulation. While banned in the United States since 1969 due to early toxicity scares, Cyclamates remain widely approved and safely used in over 100 other countries, including parts of Europe and Canada, illustrating how regulatory stances can sometimes diverge from the evolving scientific consensus.
The Ubiquity of the Illusion
These compounds have permeated our food supply far beyond the obvious can of diet soda. While zero-calorie beverages remain the primary vehicle for consumption, delivering potent doses of Aspartame or Ace-K, the “sugar-free” label has expanded into every aisle of the supermarket. We find them in “guilt-free” desserts, diabetic-friendly chocolates, and low-calorie condiments. Perhaps most relevant to the younger, health-conscious demographic is the fitness industry. Almost all whey protein isolates, pre-workout formulas, and branched-
chain amino acid supplements rely heavily on Sucralose to keep carbohydrate counts low while masking the naturally unpleasant, bitter taste of amino acids and minerals. Even the pharmaceutical industry utilizes these agents in cough syrups, chewable vitamins, and liquid medications to improve palatability, subtly training our palates to expect sweetness even in our medicine.
Mechanisms of Action: The Biological Ghost
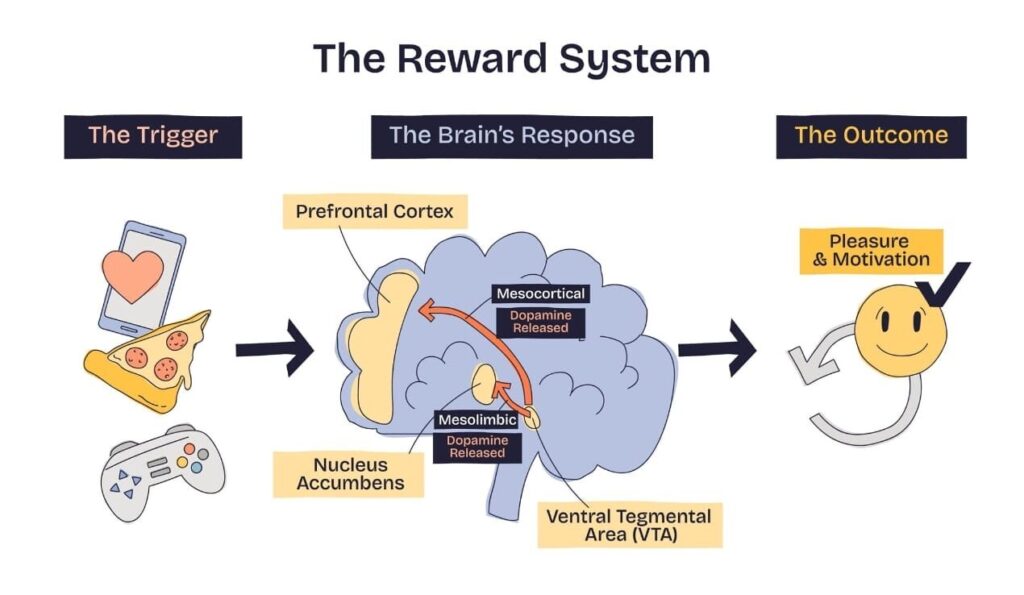
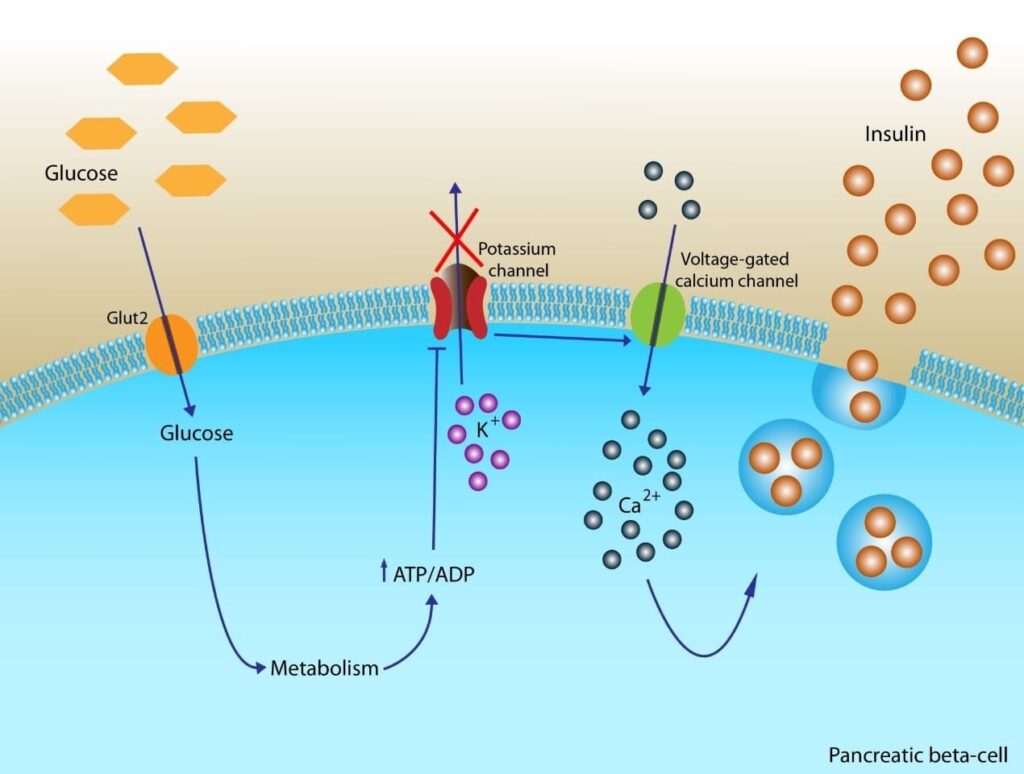
When an artificial sweetener hits the tongue, it binds to the T1R2/T1R3 sweet taste receptors. This binding sends an immediate, potent signal to the brain’s reward center, specifically the nucleus accumbens, releasing dopamine. The brain perceives sweetness and anticipates a rush of calories to follow. This anticipation can trigger a physiological reflex known as the Cephalic Phase Insulin Release (CPIR). In this priming mechanism, the pancreas releases a small burst of insulin to handle the expected sugar. When that sugar never arrives, the circulating insulin has nothing to act upon.
While this does not happen in every individual or with every sweetener, the concern is that chronic repetition of this cycle, ie: high insulin with low glucose, may theoretically contribute to a downregulation of insulin receptor sensitivity. Furthermore, the metabolic machinery operates on prediction. By consistently breaking the promise of calories, we may be degrading the predictive relationship between taste and nutrient content. This confusion is hypothesized to lead to compensatory eating, where the body drives the individual to seek the calories it was promised but didn’t receive, creating a cycle of dissatisfaction and hunger.
The Invisible Organ: Impact on Gut Microbiome
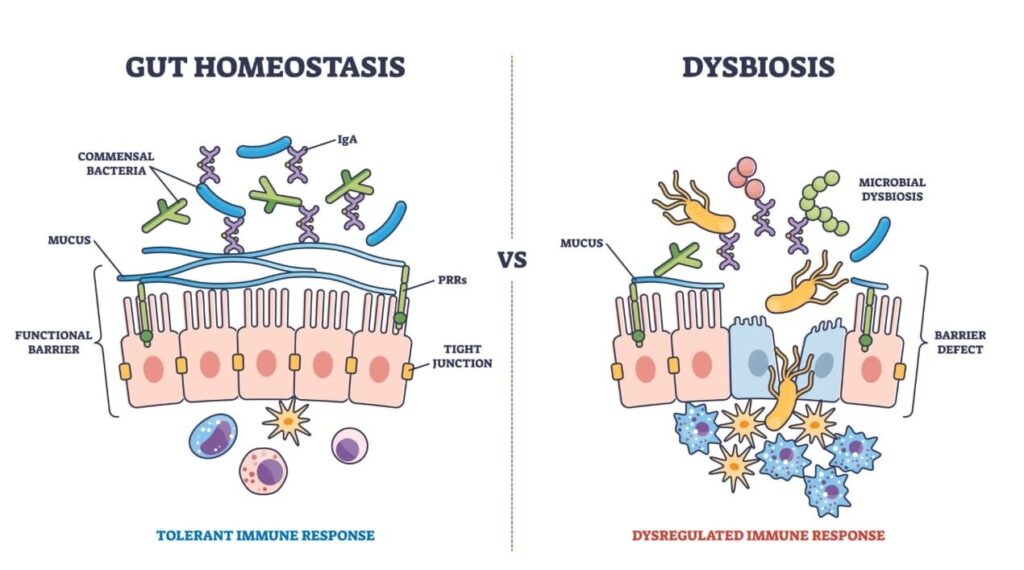
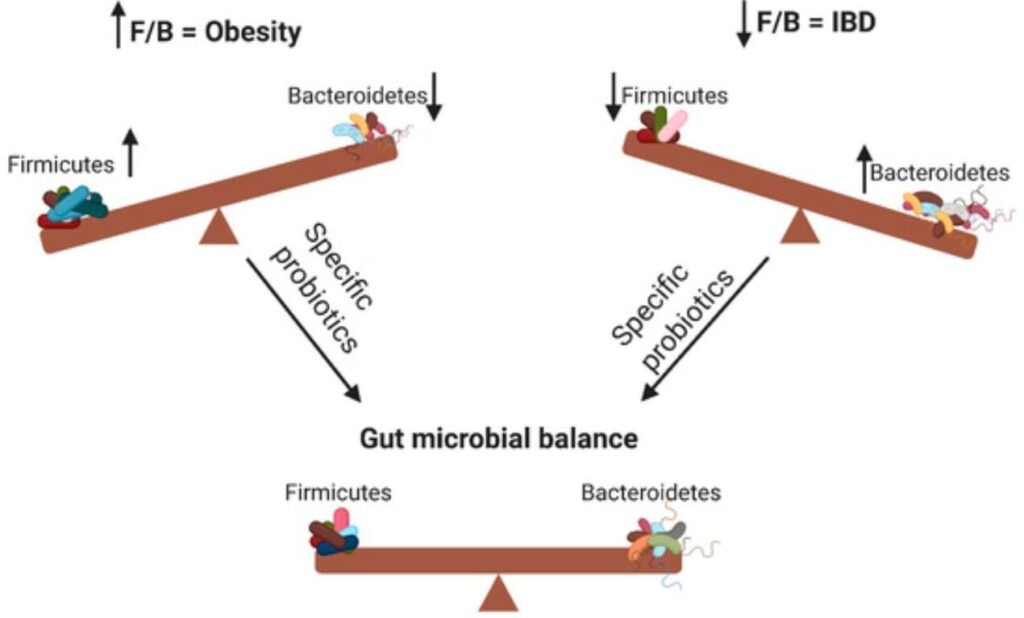
Perhaps the most disturbing evidence comes from the interactions within the “invisible organ”: the gut microbiome. Recent evidence suggests these sweeteners are not biologically inert as they pass through the intestine. Compounds like Saccharin and Sucralose have been shown to alter the composition of gut microbiota, specifically shifting the bacteroidetes/firmicutes ratio.
This dysbiosis has functional consequences. Animal studies indicate that this shift in bacterial population can induce glucose intolerance. The altered bacteria may become more efficient at harvesting energy from the diet or may trigger low-grade systemic inflammation, mimicking the pathophysiology of early diabetes. The sweetener passes through us, but it leaves a footprint on the ecosystem within us.
The Weight Loss Paradox
The ultimate question still remains: Do artificial sweeteners actually lead to weight loss? The evidence is frustratingly inconsistent, largely because they can disrupt appetite regulation. Sweeteners break the brain’s predictive link between sweet taste and calorie intake. When the expected “fuel” doesn’t arrive, the user may feel unsatisfied, potentially driving “compensatory eating”, which translates to a later craving for more carbohydrates to fill the void.

Additionally, the “Health Halo” effect contributes to this problem. People often justify consuming more high-calorie food because they feel they’ve “saved calories” by choosing a diet drink. This behavioral compensation frequently cancels out any calorie deficit created by using the sweetener.
Systemic Effects and Safety
It’s not just about weight, though; there are also worries about how these sweeteners affect our blood vessels and brain. Some studies that just observed people have tentatively suggested that drinking a lot of artificially sweetened drinks might increase the risk of high blood pressure and stroke. This could be because they might trigger inflammation or mess with how the inner lining of our blood vessels (the endothelium) works. As for the brain, some sensitive people have reported getting headaches or mood swings after taking high doses of aspartame. Scientists think this might be due to changes in neurotransmitters, but whether there’s a strong, direct cause-and-effect relationship is still a topic of intense scientific discussion.
Regulatory bodies like the FDA and WHO give these sweeteners their stamp of approval, deeming them “safe” within certain boundaries, calling them the Acceptable Daily Intake (ADI).
But here is the crucial, chilling truth: in the cold language of regulators, “safe” merely means the compound won’t poison you or kill you right away. It offers no guarantee that it is harmless to your metabolism or truly “healthy” for your long-term body chemistry. Something can be deemed “safe” to swallow, yet still subtly, fundamentally disrupt the optimal working of your internal systems.
The Path Forward
Replacing sugar with chemicals is a temporary band-aid, not a cure. The ultimate goal should be Taste Retraining. The human palate is malleable. By gradually reducing the intensity of sweetness in our diet by diluting diet drinks, reducing sweetener tablets, we can reset our baseline. Within two weeks of low-sugar intake, the taste buds upregulate their sensitivity. Suddenly, natural foods like fruit taste intensely sweet, and the chemical mimics taste cloying and artificial.

The zero-calorie promise is seductive, but biology keeps score. While artificial sweeteners are a useful tool for transition or for severe diabetics who need immediate glycemic control, they are not a free pass. They maintain the addiction to sweetness, potentially disrupt the gut microbiome, and confuse hormonal signaling. The principles of Minimal Interference Nutrition suggest that the best diet is one the body understands, and the body understands real food, not synthetic mimics.
Artificial sweeteners are tools, not food. They may help as a short-term bridge for a severe diabetic addiction to soda, preventing acute hyperglycemic crisis. They likely harm when used as a daily water replacement for a lifetime, disrupting the gut and the brain’s reward systems. The best diet follows the principle of minimal interference nutrition: communicate clearly with your body. Eat real food. Drink water. And if you must have sweetness, let it come from a fruit or a touch of honey, not a laboratory experiment