Azal was a happily married woman and a mother who had been leading a stable life. Over time, she began to feel unusually distressed and started hearing voices that nobody else could hear. She also developed strong fears and apprehensions that people around her were trying to harm her. These experiences gradually affected her behaviour and her sense of safety at home. Such changes in perception, thoughts, and behaviour hampered her daily life. Well, what really happened to her? What changed? What might be the cause? Will Azal ever be able to recover? Keep reading to know more…

SCHIZOPHRENIA: A Conceptual and Clinical Overview
Schizophrenia is a severe, chronic mental disorder that disrupts how a person thinks (thoughts), feels (perceptions) and behaves . People often present through symptoms like hallucinations (seeing/hearing/smelling and feeling things which are not real) and delusions (false beliefs) and lose touch with reality and can also present with low mood and reduced activity and self care.
As per the Diagnostic and Statistical Manual of Mental Disorders (DSM-5 TR) criteria, schizophrenia involves a range of cognitive, behavioural,and emotional symptoms. Schizophrenia is not the same as split personality disorder or multiple personality disorder and living with it does not make you a dangerous or aggressive person.
Prevalence:
Schizophrenia and spectrum disorders prevalence is around 1 to 1.4 % among the population and this slightly varies in different countries based on the diagnostic criteria adopted. Although it is not as common as other mental disorders it is important to be well aware of the disorder to catch onto early signs to prevent increasing severity of the disease. According to global burden of disease study (2017): 3.5 million people were affected in India.
Usually, schizophrenia develops in three phases:
1. Prodromal phase: Initial phase where people around you start to notice subtle changes in your behaviour and thinking. This phase can last from weeks to years.
2. Acute/Active phase: This stage could be the most alarming as it includes symptoms of psychosis such as delusions, hallucinations, speech impairment, and social anxiety. Sometimes this phase appears without a prodromal phase.
3. Residual phase: Generally 1/3rd have good recovery ,1/3rd have medium recovery and the rest 1/3rd will have ongoing residual symptoms. Adequate support, aid, and uninterrupted therapy help to improve your symptoms.
SIGNS AND SYMPTOMS OF SCHIZOPHRENIA
When does it usually begin?
The DSM-5 reports that schizophrenia symptoms typically become apparent at ages 18-35. Onset prior to adolescence is rare. The peak age at onset for the first psychotic episode is in the 20-25s for males and 26 and up for females. Onset may be abrupt, appearing virtually overnight, or insidious, unfolding over several weeks or months. Depressive symptoms are reported in about 50% of cases.
Early Signs of Schizophrenia: Recognizing the Red Flags

Though the early signs and symptoms of schizophrenia differ from person to person, these are certain common early signs that can help to alert the possibility of a psychotic disorder. The signs thus observed include:
- Social Withdrawal and Isolation
- Sleep Disturbances
- Changes in Eating Habits
- Inability to Concentrate or Focus
- Unexplained Irritability or Anger
- Unexplained Physical Ailments
- Lack of Personal Hygiene
- Decline in Academic or Occupational Performance
- Heightened Anxiety or Paranoia
Above are examples of subacute symptoms that most teen parents report. Although having one or two such symptoms is totally normal at that age, if you are experiencing anything like this that is hampering your day-to-day activities and disturbing your mental health, then an appointment with a psychiatrist is recommended.
SIGNS AND PHASES OF SCHIZOPHRENIA:
What are the symptoms associated with Schizophrenia?
According to DSM-5 there are five key signs and symptoms that characterize schizophrenia:
(1) hallucinations
(2) delusions
(3) disorganized speech, for example, loose associations
(4) disorganized behavior (which may manifest as catatonia)
(5) negative symptoms such as apathy, abulia, and anhedonia.
Positive and Negative symptoms in Schizophrenia:
POSITIVE SYMPOTOMS: Positive symptoms refer to the exaggerated thoughts, behaviour and perception which makes it nearly impossible for the person to differentiate from what is real. These symptoms are not normally present and are hence additional to what the person is usually like.
Some of the positive symptoms include:
- Hallucinations – false perceptions (types include auditory, visual, tactile, olfactory and gustatory)
- Delusions – false beliefs (some common examples are delusion of persecution, reference, control, grandeur, jealousy, poverty, misidentification, guilt etc)
- Disorganised thinking
- Distorted speech
NEGATIVE SYMPTOMS: Negative symptoms of schizophrenia reduce or “take away” from someone’s personality leading to a reduction or absence of normal behaviour and emotions.
Negative symptoms consist of five key areas:
- Difficulty expressing emotions, e.g., diminished facial expressions (called blunted- or flat affect)
- Reduction in the number of words spoken (alogia)
- Reduced goal-directed activity due to decreased motivation (avolition)
- Reduced social activity (asociality)
- Reduced experience of pleasure (anhedonia)
Exclusion of other causes of disturbed behaviour:
Clinicians have to rule out other physical health causes like delirium , infections etc which could have possibly caused disturbed behaviour. At times, substance abuse or alcohol misuse may contribute to similar symptoms.
Diagnostic approach to Schizophrenia
To receive a diagnosis of schizophrenia, a person must have experienced at least two of the following symptoms for a period of one month, with some level of disturbance being present for over six months.
Diagnosis of Schizophrenia include:
- Physical Examination of the patient where the doctor assesses general appearance, including hygiene and grooming, looks out for signs of substance abuse or skin infections.
- Blood tests may help rule out other conditions such as substance abuse or alcohol misuse that may contribute to similar symptoms
- Mental health evaluation where a physician observes the patient’s behaviour, speech, psychomotor activity, psychosocial activity, cognition and judgement.
- MRI: Although it cannot definitively rule out schizophrenia but it helps us to rule out other causes that might be leading up to similar neurological symptoms.
Determinants of Schizophrenia: A Critical Overview
Although the definite cause of Schizophrenia is yet to be confirmed, research suggests a combination of physical, genetic, psychological and environmental factors can make a person more likely to develop the condition.
Genetics: You are more likely to develop schizophrenia if it runs in your family.
Neurotransmitters: Neurotransmitters are chemicals that carry messages between brain cells. As per research, imbalances in neurotransmitters, primarily dopamine and glutamate, disrupt brain cell communication leading to Schizophrenia.
Drug abuse: Studies have also suggested that drug abuse, particularly cannabis, cocaine, LSD or amphetamines, can increase the risk of developing schizophrenia or psychosis by disrupting your neurotransmitter levels.
Stress: Stressful or emotional life events might trigger a psychotic episode. Research suggests that stress due to discrimination, work stress and stress due unemployment particularly among immigrants could lead to development of schizophrenia even without any genetic predisposition.
Pregnancy and birth issues: such as not getting enough nutrition before or after birth, low birth weight, or exposure to toxins or viruses before birth that may affect brain development.
Environment: Environmental factors that have been repeatedly investigated and often associated with Schizophrenia include obstetric complications, infections, winter or spring birth, migration, urban living, childhood adversity and weather changes.
Complications caused by Schizophrenia:
1. Suicide attempts and thoughts of suicide. (If a person is in danger of suicide or has made a suicide attempt, make sure that someone stays with that person SUICIDE HELPLINE NUMBER: Call 9152987821)
2. Anxiety disorders and obsessive compulsive disorder, also known as OCD.
3. Depression.
4. Misuse of alcohol or other drugs, including nicotine.
5. Not being able to work or attend school.
6. Money problems and homelessness.
7. Social isolation.
8. Health and medical problems.
9. Being victimized.
10. Aggressive or violent behaviour, though people with schizophrenia are more likely to be assaulted rather than assault others.
Is it true that life expectancy is decreased in schizophrenia?
Schizophrenia decreases life expectancy by between 10 and 28 years. This is primarily because of its association with heart disease, diabetes, obesity, poor diet, a sedentary lifestyle, and smoking. Suicidal thoughts followed by attempts also become a reason for decreased life expectancy.
Treatment and management: “There is hope”
Schizophrenia requires lifelong treatment, even when symptoms have subsided. Treatment with medications and psychosocial therapy can help manage the condition.
A psychiatrist experienced in treating schizophrenia usually guides treatment. The treatment team also includes a psychologist, social worker, psychiatric nurse and possibly a case manager to coordinate care.
Medications:
Antipsychotic medications are the most prescribed drugs that are combined with psychosocial interventions and social support. Other medications such as antidepressants or anti-anxiety drugs may also help. It can take several weeks to notice an improvement in symptoms.
It is important to continue your medications even after your symptoms get better to avoid relapse. It’s also important to take part in psychosocial treatments, including:
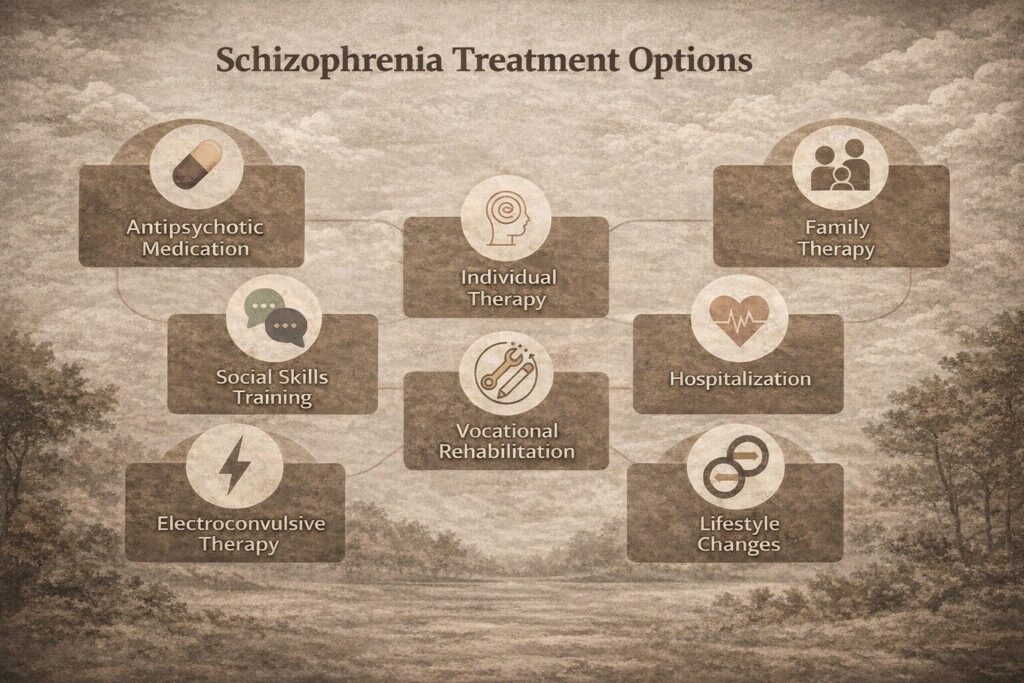
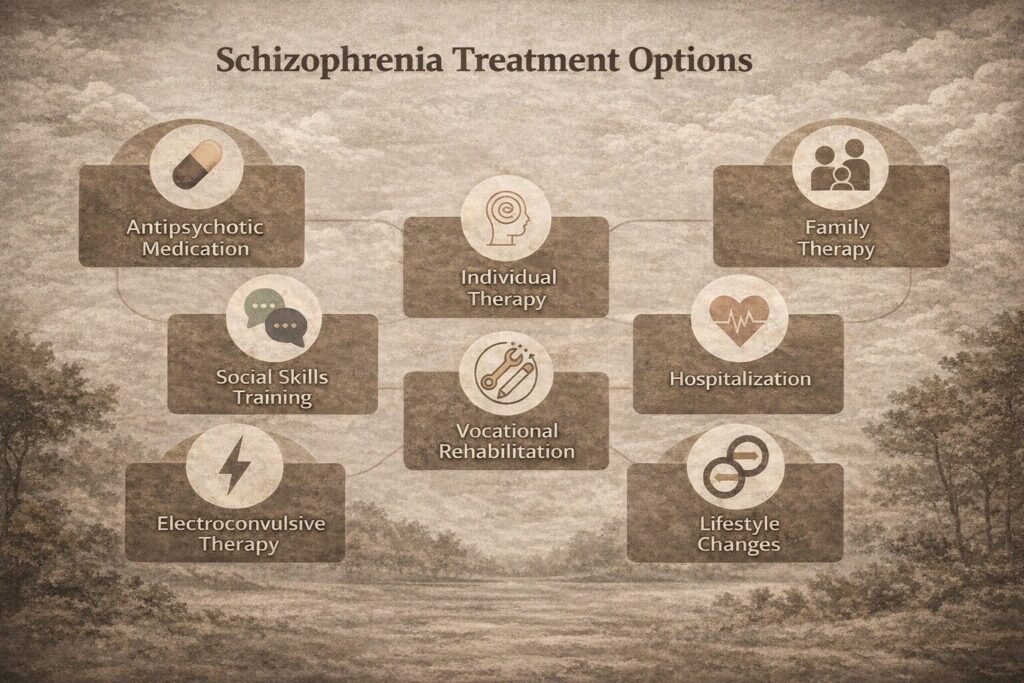
- Individual therapy: includes relaxation exercises, psychoeducation, self-reflection, self-awareness and individuals” vulnerability to stress.
- Art therapies: where he/she can let their feelings out by drawing and painting this also enables them to communicate better.
- Cognitive training: (recent advances) in which there is utilization of computer-generated exercises, here neural networks are influenced in such a way that cognition and working memory is improved.
- Social skills training: This focuses on improving communication and social interactions and improving the ability to participate in daily activities.
- Family therapy: It primarily focuses on educating the family about the immediate situation and how to approach them. Therapists also direct the family on how to take care of the patients and tell them effective ways to reduce relapses. Prevent showing high expressed emotions.
- Vocational rehabilitation and supported employment: which include joining clubs, workshops and provision of temporary employment programs.
Up to 30% of people with schizophrenia don’t react well to medications. In such cases, ECT might be necessary.
Hospitalization in schizophrenia is necessary when there is:
- Risk to self
- Risk to others
- Severe psychotic symptoms
- Inability to function socially or occupationally
- Noncompliance to treatment
- Need for intensive treatment
Some myths and stigma associated with Schizophrenia
Schizophrenia is one of the most stigmatised mental disorders. This is due to myths, misinformation and negative portrayals of the disorder by the media. These myths in turn cause fear, discrimination and poor treatment outcomes for the patient.
Myths:
Myth 1: All people with Schizophrenia are violent and dangerous:
Although some people with schizophrenia are violent, most of them aren’t. They are more likely to be victims of violence than perpetrators.
Myth 2: Schizophrenia can’t be cured:
Many patients significantly recover with early diagnosis and treatment with proper management. The key is to take medications regularly even after recovery until the doctor advises otherwise to prevent relapse.
Myth 3: Schizophrenia is caused by bad omen or bad parenting or sin of the past:
It is a biological brain disorder involving genetic vulnerability, neurotransmitter imbalance and other environmental factors.
Myth 4: All patients have the same symptoms:
Schizophrenia has a wide variety of symptoms, and each person tends to have a different set of symptoms.
Myth 5: People with schizophrenia can’t work or study:
With proper treatment and support they can work, study and live independently.
Stigmas:
Public stigma (labelling the person as mad/dangerous) – leads to social rejection, unemployment and marital issues.
Self-stigma (believing all the negative stereotypes) – leads to low self-esteem, depression, poor adherence and suicidal risk.
Family stigma (blaming and avoiding) – causes delayed treatment and counselling of the illness.
Schizophrenia vs Psychosis: Understanding the differences

Psychosis refers to a condition wherein a person loses touch with reality. It’s one among the several symptoms of schizophrenia, a mental health disorder. But people who do not have schizophrenia can also experience psychosis.
When a person experiences psychosis for a significant period of time (for nearly a month with active symptoms) and is also experiencing functional impairment, schizophrenia may be the resulting diagnosis.
Experiencing a psychotic episode does not necessarily mean a person has schizophrenia. A doctor usually rules out other possible causes before making a diagnosis of schizophrenia or other mental health condition. Although the treatment options for psychosis and schizophrenia are generally similar, early diagnosis can greatly improve the outlook and provide a better prognosis. So be sure to seek medical advice if you or your loved one has any signs of psychosis or schizophrenia.
Hope through Understanding: Conclusion
From the above article we can infer that Azal was suffering from schizophrenia. She underwent the necessary treatment and took medications regularly as advised by the doctor. She got better with time and her symptoms improved. There’s always a chance of relapse if the medications are discontinued,but with adherence there is no stop for recovery. This proves that even shattered minds can mend.
Schizophrenia does not define a person—it reveals their resilience. Every day lived is an act of courage, every step forward a quiet victory. With compassion, understanding, and the right support, moments of clarity, joy, and connection continue to grow. Life may unfold differently, but it is no less meaningful. There is beauty in persistence, strength in vulnerability, and hope in knowing that no one walks this journey alone. Each person is more than their illness: they are worthy, capable, and deeply human.
REFERENCES
Schizophrenia, an overview: American Psychiatric Association. What Is Schizophrenia?. Psychiatry.org, American Psychiatric Association. Available at: https://www.psychiatry.org/patients-families/schizophrenia/what-is-schizophrenia
Prevalence and Statistics: National Institute of Mental Health. Schizophrenia: Statistics. U.S. Department of Health and Human Services, National Institutes of Health. Available at: https://www.nimh.nih.gov/health/statistics/schizophrenia#part_2546
Symptoms of Schizophrenia: Cleveland Clinic. Schizophrenia. Cleveland Clinic Health Library. Last reviewed August 13, 2025. Available at: https://my.clevelandclinic.org/health/diseases/4568-schizophrenia
Diagnostic approach : Hany, M., & Rizvi, A. (2024). Schizophrenia. In StatPearls [Internet]. StatPearls Publishing. National Center for Biotechnology Information (US), Bookshelf. Available at: https://www.ncbi.nlm.nih.gov/books/NBK539864/
World Health Organization. Schizophrenia: Fact sheet. WHO News Room, World Health Organization. Last updated 6 October 2025. Available at: https://www.who.int/news-room/fact-sheets/detail/schizophrenia
Wikipedia contributors. Schizophrenia – Management, in Wikipedia, The Free Encyclopedia. Available at: https://en.wikipedia.org/wiki/Schizophrenia#Management
Cleveland Clinic. Schizophrenia. Cleveland Clinic Health Library. Last reviewed August 13, 2025. Available at: https://my.clevelandclinic.org/health/diseases/4568-schizophrenia
Can ECT help treat schizophrenia: Pedersen, T. (Medically reviewed by Yalda Safai, MD, MPH). ECT for Schizophrenia: Benefits and Risks. Psych Central. Published September 6, 2022. Available at: https://psychcentral.com/schizophrenia/ect-for-schizophrenia
Psychosis vs Schizophrenia: Washington, N., DO, MPH (Medically reviewed) & Seladi-Schulman, J., Ph.D. (Writer). Psychosis vs. Schizophrenia: Understanding the Difference. Healthline. Updated June 25, 2025. Available at: https://www.healthline.com/health/schizophrenia/psychosis-vs-schizophrenia
Fletcher, J. Psychosis vs. Schizophrenia: How Do They Differ? Medically reviewed by Yalda Safai, MD, MPH. Medical News Today, updated May 6, 2025. Available at: https://www.medicalnewstoday.com/articles/psychosis-vs-schizophrenia#psychosis-vs-schizophrenia


